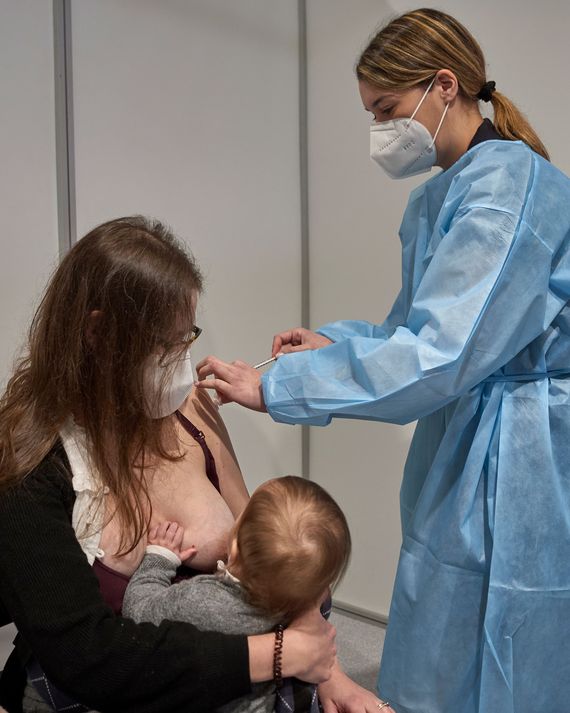
In early March, Jordana Gorsky was the only fully vaccinated member of her household. A speech-language pathologist, she was required to report to work in person. But when her kids’ au pair brought home the coronavirus, she believed at least one other member of the family would be protected.
“I was so certain the baby would not get it,” Gorsky says of her then-10-month-old. He was still breastfeeding, and she had read about studies that had found antibodies in vaccinated parents’ breast milk. “I really put all my eggs in this basket of antibodies passing through the breast milk.” Unfortunately, both of her sons tested positive, and the baby was, she said, “pretty sick,” with high fever, fatigue, and congestion. Both boys recovered within about a week.
Gorsky wasn’t alone in hoping breast milk from a vaccinated person would immunize babies or children who can’t yet get the shot. So did the parents on the underground market for vaccinated breast milk that sprang up seemingly overnight, and the women who, according to the New York Times, “swarmed” support groups for relactation, trying to get their bodies to restart milk production by hooking themselves up to an electric pump every two hours. One woman told New York that her friend had snuck her donated milk into scrambled eggs for her 4-year-old twins and 9-year-old in hopes of protecting them.
The truth is that while researchers have found preliminary evidence that COVID-vaccine antibodies in human milk can neutralize the virus in a lab, such passive immunity is far more complex and contingent than a lot of the coverage has suggested — especially after the first few months of a child’s life. “The protection offered by passive transfer through mother’s milk is not like a vaccine, where we’re generating the baby’s own immune response,” says Lori Feldman-Winter, a professor of pediatrics and chair of the American Academy of Pediatrics’s Section on Breastfeeding.
Scientists have offered these kinds of caveats all along, but you have to read pretty far down in a lot of the articles to find them. An April New York Times article, for example, declared that “newly vaccinated mothers are right to feel as if they have a new superpower,” but took 15 paragraphs to get to an expert saying the protection may be only partial.
Because lactating and pregnant people were excluded from the vaccine clinic trials, experts were understandably eager to rebut fears that the shots wouldn’t be safe for them, and to tout the added benefits. Rebecca Powell, a professor at Mt. Sinai whose research focuses on infectious diseases and human milk, told me she thought that in contrast to the negative framing in a lot of COVID-19 coverage, “this is a case of, let’s focus on something good that is also interesting and worth talking about.”
But the optimistic reports have also left parents like Melanie Olson understandably confused. A teacher in New Jersey, she was nine days past her second shot when her breastfed 11-month-old became quite ill with the coronavirus. His pediatrician gave the baby a steroid treatment and told his parents that hospitalization might be necessary, but luckily his condition improved overnight. (Both Olson and her two older sons repeatedly tested negative.) “It’s a disappointing feeling, because it’s not like breastfeeding comes easy to anyone,” she said. “It made me feel like, okay, this did nothing.”
Of course, as Powell points out, we have no way of knowing how many infections didn’t happen because of the antibody protection offered by lactation among the vaccinated. And, says Feldman-Winter, these babies may have benefited from their exposure to breast-milk antibodies even if they still became very ill. “I would wonder if even there was some protection offered where otherwise it could have resulted in more severe disease,” she said.
To understand why these babies got sick at all, it’s helpful to understand that so-called passive immunity is more of a spectrum than a light switch. Babies are born vulnerable with immature immune systems, but they can get one layer of protection from maternal antibodies passed through the placenta, including naturally acquired ones (from sickness) or ones acquired from vaccines. That’s one reason why flu and whooping-cough vaccines are recommended late in pregnancy. Those antibodies typically last the first few months of a baby’s life.
Breast-milk antibodies are different in both function and composition. Rather than enter the bloodstream, says Yariv Wine, an immunologist at Tel Aviv University who is conducting research on the breast milk of vaccinated parents, these antibodies “aim to especially protect the entry points to the body. They target what we call mucosal tissue — the respiratory tract, our oral cavity, our gut lining.”
That COVID-19 is a respiratory virus has made researchers optimistic about breast milk’s effects. But there are lots of ways this process can be diluted. First of all, Wine noted, the vaccine itself is highly effective, but it’s not 100 percent effective even in those who have received it directly. It’s easy to forget that the stated goal of the vaccines was preventing “severe disease,” not eliminating infection. Indeed, Gorsky herself tested positive for the virus, with mild symptoms, despite being fully vaccinated.
And immune response in milk itself varies by person. “One possibility is that the vaccine did not induce a sufficient level of antibodies in the breast milk,” said Wine. “We saw women in our study cohort for whom the levels of antibody in the breast milk were reduced compared to other women,” about one or two out of ten.
“The other question is how much viral load was the baby exposed to when he was infected,” Wine continued. Someone sick with COVID sneezing directly on a baby, for example, would probably inflict a lot of viral load. “It’s a balance between how much antibody is present,” he said, “and how much you get from the mother and how strong the contact was between the virus and the baby.”
That these babies were close to a year old also may matter. By six months, babies are typically eating solid foods along with breast milk or formula. “A newborn whose diet is entirely human milk — that protection is much greater than in an older infant who may be having a diet that is at least half other complementary foods,” says Feldman-Winter.
As a child grows, Powell says, the milk itself doesn’t change in its dosage of antibodies, but in wealthy countries, babies are usually taking in less. “If you have a 2-year-old who breastfeeds quite a lot, which many do in low-income countries, they may be breastfeeding seven to eight times a day,” she says. “But if you have a 2-year-old who is breastfeeding once a day at night or something, that efficacy is going to be highly reduced.” At the same time that these babies are taking in less breast milk, they’re also getting bigger themselves, a ratio that Wine says likely means antibodies are doing less.
You can’t blame desperate parents for hoping. For those who are already breastfeeding, even a reduced chance of protection is an added benefit when vaccines for younger children and babies are still in clinical trials, at least months away from approval, if that. But it’s not a silver bullet, which is what Olson wanted other parents to know before they spend hours trying to relactate or give their babies the milk of a stranger (which the FDA and the AAP already don’t recommend). “If you’re one of these people who is going crazy and struggling to pump, even though it’s killing you, or you’re already weaning, you need to hear from me,” she said. “I’m still breastfeeding, and my child still got it.”
Kathryn Gray, a maternal fetal medicine specialist at Brigham and Women’s Hospital who recently published research on vaccine response in pregnant and lactating women, says this is all the more reason to keep up other mitigation measures. “When we can actually give vaccines to kids and infants,” she says, “they’ll have better protection than any of the measures we’re able to do now.”
One thing is already clear: Breast-milk scrambled eggs won’t help. Wine says that while freezing and thawing milk is fine, at the level of heat involved in cooking, “it will ruin the antibodies.”






























